The Cancer Family Link: How Worried Should I be About Breast Cancer?
Most women know that if your mother has been diagnosed with breast cancer, you are at higher risk. But what if your mom is fine but your maternal grandmother died of breast cancer in her 30s? What if your maternal aunt died of breast cancer in her 40s? Are you at risk even if your mom is cancer-free? Or what if your dad has prostate cancer – does that matter? Dr. Michelle Walters, a Medical Director of Breast Imaging and a board certified MRI and mammography radiologist at RAYUS Radiology in Texas, gets questions like these all the time. Family history can be a strong predictor, not just for breast cancer, but for pancreatic, ovarian, prostate and colon cancer.
The technical term is familial syndrome or familial cancer. Scientists have been able to connect the dots between certain types of cancer that have a hereditary link. The genetics can be a predictor, but they aren’t a guarantee. For example, Dr. Walters says, “Just because you have the breast cancer gene does not mean you’re going to get breast cancer. It just means you’re at higher risk of getting breast cancer.” Here is research to back her up:
- Inherited gene mutations account for only 5-10 percent of all breast cancers diagnosed in women in the U.S. –American Cancer Society
- Only about 13 percent of women diagnosed have a first-degree female relative (mother, sister or daughter) with breast cancer. –The Lancet
What can you do?
Understanding your family history is the first step. Passing that information on to your doctor is the crucial second step. Once you share your family history your doctor will be on the lookout for familial cancers. In the case of breast cancer, to be certain whether you are a carrier requires genetic testing. The genetic counselor looks for an abnormality in your gene that indicates BRCA1 or BRCA2.
Think it will be too stressful to get the genetic results? After researching women who went through BRCA testing, NIH’s National Cancer Institute found that both patients who were carriers of the BRCA gene and those who were not showed low levels of psychological distress in the long term from knowing the results. It might seem scary to take that step, but if you are armed with the best information, you can make the best choices about your health.
Monitoring with MRI
If you have an elevated risk of developing breast cancer, you have options. Some women with the BRCA2 gene opt for a mastectomy. Actress Angelina Jolie spoke publicly about her decision to have a bilateral mastectomy after her doctors told her she had an 87 percent risk of breast cancer. Other women decide to take preventative steps by closely monitoring their breasts with routine imaging.
When asked if breast MRI is a good way to screen for breast cancer, Dr. Walters says, “Absolutely! MRI is the most sensitive test we have for breast imaging. It’s a great test because it’s 98-99 percent sensitive for breast cancers.” For high-risk women, getting an annual breast MRI is the best way to look into the tissue of your breast and make comparisons from year to year.
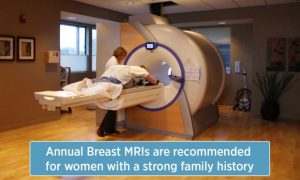
The American Cancer Society backs that up, recommending if you have a primary relative – a mother, sister, brother or father – with the breast cancer gene, you should get yearly MRIs. That also means monitoring your breasts at a younger age. If you have a strong family history, the National Comprehensive Cancer Network recommends that starting at age 30 you get a:
- Clinical breast exam every 6-12 months
- Mammogram every year
- Breast MRI every year
You can’t control your genes, but you can control your risk factors. If you do your hereditary homework and follow the screening guidelines, your chances of early detection are strong. When it comes to breast cancer, Dr. Walters says finding it early is key. “If you catch it really early and you treat it, then it’s curable.”
To learn more about what to expect from a breast MRI, click here.